This disease is called equine monocytic ehrlichiosis, but because it was first documented in the Potomac River Valley of Maryland in 1979, most horsemen know it as Potomac horse fever.
It has now been diagnosed in nearly every U.S. state, every Canadian province, Europe and South America.
PHF probably existed before 1979 and in other areas: “River valley fever” and “Shasta River crud” have been a problem in northern California for a long time.
Affected horses developed diarrhea, fever and usually died unless treated with tetracycline – the same drug currently used to treat horses with PHF. It just happened that a virulent strain emerged in 1979 in Maryland and gained attention and a name.
Dr. Katherine Wilson, clinical assistant professor for large animal medicine, Virginia-Maryland Regional College of Veterinary Medicine, says the disease is caused by a bacterium formerly called Ehrlichia risticci, but its name has been recently changed to Neorickettsia risticci.
“The bacteria infect a certain type of fluke that parasitizes aquatic snails and slugs,” she says. At first people thought the disease was transmitted to horses via biting insects, since this pathogen belongs to the same family of bacteria that cause tick fever. Then scientists discovered that snails were involved in the process.
“For many years, we thought horses had to eat the snails and slugs to get the bacteria, and that only horses with access to running water would be at risk. But PHF often occurs in horses that are not near water.
Then these bacteria were also found inside aquatic insects like mayflies and caddis flies. We suspect horses are being infected by ingesting the insects.
These aquatic insects can be attracted to lights around the barn and fall into water troughs or into feed,” says Wilson.
The disease
“Once a horse is infected, it may take one to three weeks to come down with the disease,” says Wilson. PHF has variable clinical signs. The classic situation is a horse going off feed, with diarrhea and fever.
Dr. Amy Johnson with the New Bolton Center in Pennsylvania, says high fever is the most consistent sign. “We see temperatures from 103 to 105ºF.
With fever, the horse is depressed. Mild depression and reluctance to eat may be the only signs you’d see at first, and this should be a clue to take the horse’s temperature,” she says.
“This is usually a biphasic fever, which means they have a fever, the temperature comes back down to normal, and then they develop another fever,” says Wilson. “Then many of them develop profuse diarrhea and become severely endotoxic and dehydrated, losing protein through the diarrhea.”
Johnson says about 60 percent of cases develop diarrhea. “Some of them won’t have visible diarrhea. It’s an internal diarrhea in which the colon is inflamed and losing fluid and electrolytes internally – but we are not seeing the horse produce much diarrhea.
The horse has all of the systemic inflammatory responses that you see with severe diarrhea, but not much external diarrhea,” she says. She advises horse owners to take the horse’s temperature if it goes off feed or acts depressed.
“The terrible aspect of this disease is that it frequently causes laminitis. In my experience, this is the major factor that causes us to lose these horses.
Most of them can get over the diarrhea with supportive treatment and IV fluids, but if their feet are severely compromised by laminitis, we can’t always save them,” Johnson explains.
Most of these horses are very sick. “About 30 to 40 percent develop laminitis. Most fatalities result from either not being treated or development of laminitis,” says Wilson.
“There are wide ranges of clinical signs, however. Some horses are just off feed, with fever, and may have decreased fecal output, acting a little colicky – and never develop diarrhea.
When we run blood work on them, they have a low white blood cell count, and if we test them for PHF, they test positive,” she says.
A pregnant mare with PHF she may abort. “In my experience, these mares are pretty sick and abort secondary to this disease,” says Wilson. Any horse that is dull and off feed, and certainly any horse that has profuse diarrhea, should be checked by a veterinarian.
Diagnosis
“The best way to diagnose PHF is to identify the bacteria in a sample of blood or feces. This is done with a PCR (polymerase chain reaction) test which detects bacterial DNA,” says Wilson.
The sample can be sent to a lab that does PCR tests. “We usually get test results back within a couple of days. But if we suspect the horse might have PHF, we start treating immediately, before we get the test results,” she says.
“Despite the fact that multiple horses on the farm might be exposed to PHF, usually only one horse gets sick. By contrast, if multiple horses develop diarrhea, we suspect something infectious (and contagious horse to horse) like salmonella, although I have had farms with multiple horses get PHF,” Wilson says.
“It can be confusing, because the horses may look like a mild colic or an impaction because they are dull and not passing manure. The fever would be a clue, however, because we don’t see fever in impaction cases.
If we run blood work, their white cell count is low, and that’s not typical of impaction colic, either.” In these instances, most veterinarians would start treatment, in case it is PHF.

Treatment
Horses that get diarrhea need intensive treatment and are usually best treated in a hospital situation rather than on the farm.
“It is best to treat as quickly as possible, before they get secondary complications from dehydration and become endotoxic.
This can make the prognosis worse and treatment more prolonged. The quicker we can get a horse on antibiotics, the quicker it will respond,” says Wilson.
The antibiotic most commonly used is oxytetracycline given intravenously.
“In a mild case, this can be done on the farm, but if the horse has diarrhea and is dehydrated it needs IV fluid support and other supportive care – and laminitis prevention,” she says.
Johnson says the organism is very susceptible to oxytetracycline. “Sometimes the oral form (doxycycline) is used.
In our clinic we generally use the IV formulation, since the horses we see often have GI issues.
If the GI tract is not working properly it can’t absorb the oral drug,” says Johnson.
“A person must be careful in treating these horses, because if they do have diarrhea or systemic inflammatory response syndrome, they may be dehydrated.
Oxytetracycline can be damaging to the kidneys, especially in a horse that’s dehydrated, so we frequently give IV fluids as well.
When we treat cases that are caught really early – the first day they go off feed and have a fever – we might get away with just giving the oxytetracycline IV for a few days without any other treatment, since the horse is not yet dehydrated,” she says.
“Regarding possibility of laminitis, we tend to be proactive in trying to prevent it, but laminitis is not always easy to prevent. The best situation is to treat the horse as early as possible with oxytetracyline and put it in a deeply bedded stall with soft footing.
We make sure these horses are as healthy as we can get them with IV fluids and anti-inflammatory drugs and try to ice their feet before they develop laminitis.
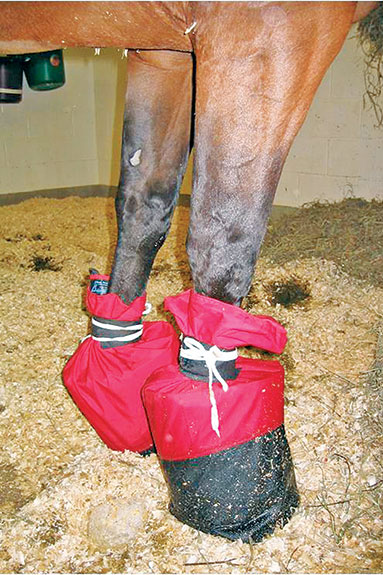
We sometimes put supportive pads on their feet.
The ice and supports may be more helpful with the type of laminitis we see with severe colic cases and some of the other diarrheas, but we still do these things to try to prevent laminitis in PHF,” says Johnson.
Prevention
In regions where PHF has occurred, horse owners should consider vaccination. “There is a vaccine available, but it is not as effective as we’d like,” says Wilson.
“It doesn’t have long duration of immunity – perhaps a couple months. There are different strains, and the vaccine only protects against one strain.
In areas where there is high prevalence of the disease, we recommend vaccinating twice – if it’s not cost-prohibitive for a farm with many horses.
We suggest vaccinating in late spring, before summer fly season and again mid-summer to give protection through the fall,” she says. That way you are vaccinating the horse in time to develop immunity but before the most risky time.
“The vaccine may not always prevent the disease, but we think it might reduce the severity of clinical signs. The vaccinated horse may have a mild case rather than severe illness that might be life-threatening.”
Other ways the disease might be prevented is to reduce horses’ exposure to aquatic insects. “One well-known farm was able to reduce the incidence of PHF in their horses by turning off their outside lights at night,” says Wilson.
“Since snails are part of the life cycle in this disease, one way horse owners might prevent PHF is to reduce snail populations in horse pastures,” says Johnson.
“This can be tricky in some regions and climates, but eliminating areas of standing water can help. Another strategy would be to get rid of the carrier insects by using insect traps,” she says. ![]()
Heather Thomas is a freelance writer based in Idaho.
PHOTOS
TOP: The first signs of PHF may be depression and reluctance to eat.
MIDDLE TOP: Treatments of IV will typically help horses with PHF overcome diarrhea.Photo by Katherine Wilson.
MIDDLE BOTTOM: Provide soft footing, as with these ice boots, to treat possible laminitis with PHF.
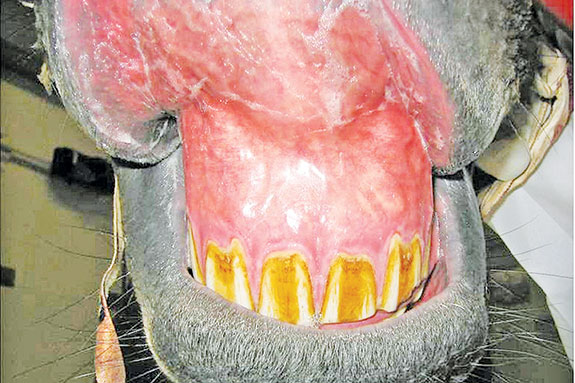
BOTTOM: The dark-colored membranes on this horse with PHF are evidence of dehydration/toxic shock from diarrhea. Photos courtesy of Amy Johnson.
Prognosis
“Published studies looking at case fatality rates vary from 5 to 30 percent,” says Dr. Katherine Wilson. “There are different strains of the bacteria, and this may determine the severity of clinical signs.
The case fatality rate may vary with the strain involved. Most of the fatalities are due to laminitis or severe endotoxemia.
Usually if a horse recovers from PHF (even if it was just a mild case) that horse is then immune to this disease for up to two years.”

Dr. Katherine Wilson

Dr. Amy Johnson








