For dairy managers dealing with metabolic issues during transition, subclinical hypocalcemia (SCH) can be one of the more frustrating challenges to overcome. It’s one of those issues you know exists, but the extent is often unclear and the impact unknown.
You can quickly spot cows with clinical hypocalcemia; however, cows with SCH are difficult to identify. That’s because cows with SCH do not show the clinical symptoms associated with milk fever. The cow’s blood calcium level has not yet fallen low enough to cause clinical milk fever, but it’s low enough to cause a cow health and production challenges. The threshold at which this occurs is still unknown.
SCH usually occurs within the first 24 to 48 hours after calving as the cow’s lactation begins.
Tip of the iceberg
This “invisibility” is one of the reasons SCH is sometimes thought of as an iceberg disorder: what lurks below the surface of what you can see can cause significant harm.
SCH negatively affects immune function, production performance and reproductive function. It also increases the risk for postpartum metabolic diseases.
For instance, researchers at the University of Florida recently quantified the cumulative effects of SCH on secondary transition health disorders and management challenges. They found that cows with SCH were more likely to have:
- A 3.2X increased risk of metritis
- A 2.4X increased risk of postpartum fever
- Increased post-fresh levels of blood beta-hydroxybutyrate (BHBA) (1 versus 0.7 mmol per L) – blood BHBA is the ketone body most commonly used to diagnose ketosis and subclinical ketosis.
- Longer median days open (124 versus 109 days)
Therefore, it’s essential you take steps to reduce the risk of SCH within your herd and address underlying causes to protect animal health, performance and your dairy’s profitability.
Widespread impact
If you’re struggling with SCH on your operation, you’re not alone.
SCH impacts a significant number of cows in herds all across the country. The National Animal Health Monitoring System (NAHMS) estimates as many as 54 percent of multiparous cows and 25 percent of first-calf heifers succumb to SCH, even though clinical cases of hypocalcemia are much lower overall and almost absent from first-calf heifers.
Experts estimate the prevalence of SCH is likely much greater than reported, and the best way to get a handle on its impact in your herd is to implement a monitoring program. This understanding paves the way for preventative actions.
Get back to the basics
There are fundamental practices you should implement to set cows up for success and minimize incidence of SCH. These include:
- Clearly define and record transition cow events: This includes difficult calvings, retained placentas, ketosis, metritis, mastitis and start-up milk production. Use this information to establish a baseline for herd monitoring so that you can assess whether your actions are successful.
- Test forages: Consistently analyze forages and byproduct commodity feeds for sodium, potassium, chloride and sulfur by wet chemistry analysis so that dietary cation-anion difference (DCAD) can be calculated.
-
Formulate the prepartum ration for a negative DCAD: Aim for a ration DCAD of -8 to -12 meq per 100 g dry matter for 21 days prepartum. This practice is proven to adequately acidify cows and help reduce the risk of clinical hypocalcemia and SCH postpartum.
As a result, more of the total blood calcium becomes available in ionized form, which reduces the risk of SCH and milk fever. Identifying the right anion source to lower DCAD while also delivering metabolizable protein (MP) is vitally important as you formulate prepartum rations.
- Monitor urine pH: Urine pH serves as a reflection of blood pH, which assesses the implementation of the negative DCAD ration. Take urine samples from cows that have been fed the close-up diet for at least five days. Consistently collect samples at the same time post-feeding, recognizing that urine pH will vary during the day. Target the urine pH levels in Table 1.
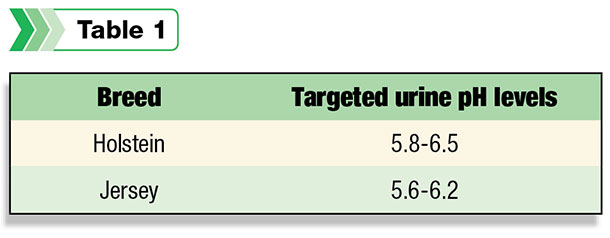
If you are adjusting DCAD to meet the targeted levels, increase or decrease DCAD until 80 percent of the cows fall in this range. Usually a DCAD of -8 to -12 meq per 100 g DM should accomplish this goal.
Follow-up monitoring
Once you’ve taken these preventative steps, you may decide to implement “before” and “after” intervention blood sampling protocols. If you do, use the following steps for optimal results.
Note: Choose animals that have consumed the close-up ration for at least five days and had a normal, uncomplicated calving. They should also be visually free of disease.
1.Draw tail vein blood from a minimum of 10 first-lactation, 10 second-lactation and 10 third- or greater-lactation animals. Take samples within the first day postpartum. This should be done after first colostrum is removed and before applying any oral or injectable calcium interventions.
2.Implement nutritional intervention.
3.After 30 days, repeat the blood sampling process as outlined in step 1 on a new set of animals.
4.Plot the before and after values by parity for each cow and compare the averages. Even without the critical threshold or ideal timing identified, this provides a true comparison to ensure the nutritional intervention was successful.
Cumulative effect
When tackling SCH on your operation, don’t forget that the benefit of carefully formulated, negative DCAD close-up diets depends on animals consuming this diet – and consuming it for an adequate amount of time. Therefore, take steps to make sure your animals have plenty of access to this diet for 21 days prior to calving.
Also consider factors like stocking density and bunk space when troubleshooting. And keep in mind that cow comfort, water quality and availability, and heat abatement all impact ration effectiveness and can play a part in SCH incidence or other health disorders on your dairy.
It’s in your best interest to take steps to ensure cows are not limited by any of these challenges that can lead to disorders like SCH that impede cow health and productivity. PD
To learn more, visit the Arm & Hammer Animal Nutrition website.

Gene Boomer
ManagerField Technical Services
Arm & HammerAnimal Nutrition






